
What is price transparency?
And how it's changing the way healthcare teams negotiate, benchmark, and grow their practices.
In 2021, CMS introduced two rules that reshaped healthcare pricing.
Hospital Price Transparency Rule
Requires all hospitals to publicly disclose negotiated rates, cash pay prices, and standard charges for all items and services in machine-readable files, plus a consumer-friendly display of 300+ shoppable services.
Transparency in Coverage Rule
Requires insurers and health plans to publish in-network negotiated rates, out-of-network allowed amounts, and drug pricing data in machine-readable files—the insurer-side counterpart to hospital transparency.
The result? For the first time ever, pricing power shifted - giving providers, analysts, and health systems access to the same contract data payers once kept behind closed doors.
ENFORCEMENT TIMELINE
Price transparency enforcement is accelerating.
What started as a publishing requirement has become a serious compliance mandate with real financial consequences.
Jan 2021
Hospital Price Transparency Rule takes effect
Jul 2022
Insurers must publish machine-readable rate files
Jan 2023
CMS begins issuing civil monetary penalties
2024
Penalties escalate to $2M/year for large hospitals
2025
Executive Order intensifies enforcement
2026
Lower Costs, More Transparency Act advances
Jan 2021
Hospital Price Transparency Rule takes effect
Jul 2022
Insurers must publish machine-readable rate files
Jan 2023
CMS begins issuing civil monetary penalties
2024
Penalties escalate to $2M/year for large hospitals
2025
Executive Order intensifies enforcement
2026
Lower Costs, More Transparency Act advances
29-55%
of hospitals found non-compliant in federal audits
PMC | Bartasian et al. 2024
$2M+
maximum annual penalties under current enforcement
CMS enforcement actions
Only 18%
of medical groups use rate data for payer negotiations
MGMA poll of 617 practices
THE DATASET
What's being published today?
Today, payers publish machine-readable files (MRFs) with negotiated rates by CPT code and provider, while hospitals publish charge masters and shoppable services in CSV or JSON formats.
This data contains trillions of rates. We download every file every month. That's more data than Wikipedia, LibGen, and Netflix combined.
95%
Commercial coverage
covering over 170M lives
10,000+
Reported insurance plans
across all 50 states
3.5M+
Healthcare providers
and organizations included
All codes
CPT, HCPCS, MS-DRG
and more…
Great, so can I go search any provider's rate in the MRFs?
Unfortunately, it's not that simple. The raw files are huge—often incomplete, poorly structured, or inconsistent. PayerPrice ingests every payer and hospital file monthly, parsing trillions of rows into clean, structured, queryable data.
We normalize rates, link them to providers by NPI or Tax ID, and layer in metadata like payer IDs and plan names — turning raw compliance dumps into usable pricing benchmarks for providers.
Speed up audits, automate your workflows, get paid accurately.
PayerPrice delivers up-to-date, contract-specific rate data in clean Excel exports or API. No guesswork. No payer delays. Just data you can use today to start recovering revenue.
Instant fee schedules
Get complete payer fee schedules in minutes. No payer portals required. Search by NPI, Tax ID, or specialty.
Keep allowables accurate
We download every rate, every month. Ensure that your fee schedules are always current, never stale.
Benchmark rates by region
Break down reimbursement by code, geography, payer, and specialty to identify negotiation opportunities.
Connect via API
Automate data extraction and revenue integrity workflows with structured rate data delivered straight to your tools.
Automate OON re-pricing
Use real contracted rates to set the usual, customary, and reasonable charges for out-of-network repricing.
Automate QPA calculation
Benchmark out-of-network qualified payment amounts (QPAs) using clean, contract-specific market data.
BEYOND COMPLIANCE
Price transparency is a strategic
asset—not just a checkbox.
Most providers treat transparency as a cost center. Leading providers treat it as a negotiation weapon.
Compliance-Only Mindset
- Publish files to avoid fines
- Minimal investment, no internal champion
- Data treated as a regulatory artifact
- No benchmarking against competitors
- Perceived as a cost center with no ROI
Strategic Mindset
- Use published data as market intelligence
- Cross-functional team owns the process
- Data fuels payer contract negotiations
- Rates benchmarked against market regularly
- Transparency becomes a revenue driver
“If I knew what my competitors' rates were, it would actually give me more leverage for higher reimbursement.”
— David Ralston, AVP Revenue Cycle, Jackson Hospital
PayerPrice aggregates data from 10,000+ health plans so providers can benchmark rates by code, payer, and region—without the manual data science burden.
Book a DemoPROVIDER STRATEGY
How providers are using price
transparency data
The 82% of medical groups not yet using published rate data are leaving negotiation leverage on the table.
Benchmark against competitors
See what insurers pay your competitors for the same procedures in the same market. Identify where you're underpaid relative to the market.
Strengthen payer negotiations
Build data-backed cases for rate increases using published benchmarks. Nine times out of 10, transparency data is now a vital piece of contract negotiation.
Identify underpayments
Surface underpayments you didn't know existed. When contracts auto renew, the gap between what you should be paid and what you are paid quietly widens.
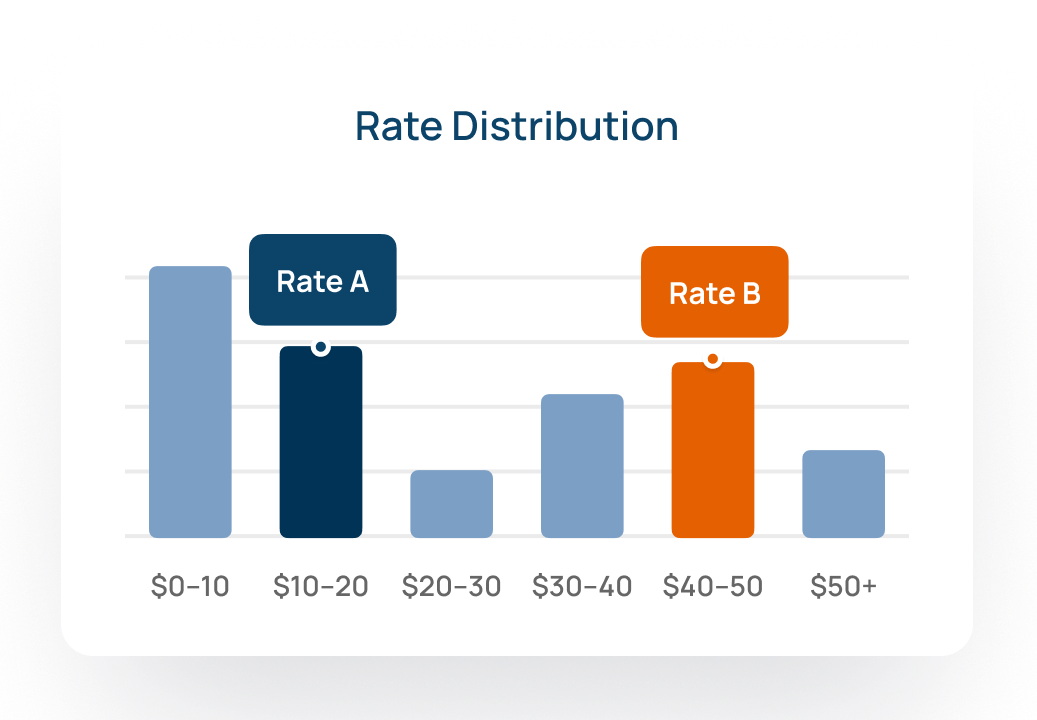
Payer Contracting & Benchmarking
Compare reimbursement rates across payers, providers, and markets to negotiate stronger reimbursement, faster.

New Market Expansion & Business Development
Understand reimbursement before entering a new market. Use payer data to support expansion, de novo builds, and diligence.

RCM, Payment Integrity, & Contract Compliance
Pull up-to-date fee schedules in seconds. Automate payment integrity and contract management at scale.
Case Study
What top negotiators achieve with PayerPrice
Identified rates below market by specialty, plan, and region
Replaced manual benchmarking with sharable presentation-ready visuals
Helped teams defend double-digit increases in payer negotiations
"Our top-line rates increased 15%"
First Name
Last Name
Company
Role / Title
Phone Number
How did you hear about PayerPrice?

